February is Congenital Heart Defect Awareness Month, so this month we will be featuring several posts from moms parenting children with heart defects. Our goal is to inform and equip those considering or home with children with this special need by sharing the real-life experiences of those already parenting a child with a CHD.
This post is written by two mamas who have walked a similar – and yet very different – path. Both of their daughters, adopted from China with complex heart defects, required what most parents would consider a worst case scenario: a cardiac transplant.
Each shares their experience below – Andrea, mom to Rini…
I am mom to six treasures, five adopted from China, four born with congenital heart disease. I am married to Eric, a small business owner. I serve as Executive Director of Little Hearts Medical, an organization dedicated to providing hope for China’s orphaned and impoverished children living with congenital heart disease through the partnership and training of Pediatric Cardiologists and Surgeons. My youngest daughter, Rini, received an angel’s heart on November 13, 2013 at Seattle Children’s Hospital.
And Emily, mom to Lily.
I am the mother to five beautiful children. I am also wife to Jacques, a Pastor at Gateway Bible Church in Gainesville, VA. In my spare time I am a Forensic Science Professor and Graduate Program Coordinator at the George Mason University. My youngest daughter, Lily Grace, received the gift of life on June 14, 2014 through heart organ donation at Children’s National Medical Center in Washington D.C.
This post will be run in two parts – there is so much wisdom shared here by these two moms, too much for a single post. Please look for the second half to be posted next week.
Cardiac Transplant: Life Springs Forth – by Andrea
“Transplant is the only option to prolong your daughter’s life.”
Those words. Cardiac Transplant. What a frightening prospect that once was to my husband and me when we first considered the adoption of a child with congenital heart disease in 2010, and yet what a blessed prospect that was three years later when we adopted our fourth CHD child.
Admitted to the hospital upon arrival to the U.S., within two weeks we learned that she was at end stage cardiac disease, inoperable, and with cardiac function so poor she was expected to survive only several more weeks even with medical support. Suddenly, a procedure that we once feared was one that we were desperate to have offered to our dying child, even more so after two centers refused to even evaluate her for transplant candidacy due to her severe malnutrition and anatomical complications.
Now that we are 15 months post transplant with our vivacious and spirited three year old, joyfully and gratefully enjoying this time of stable health, I join with my friend, Emily, and would like to share a bit about the process of transplant for those families who are considering the adoption of a child whose heart disease may lead to the need for it. Just like anything else, putting one foot in front of the other may take you to an expected and stunningly beautiful place, albeit the road leading there may be challenging. We feel absolutely blessed to be walking this road with our child!
“Always choose Hope!” – by Emily
A heart transplant is not a cure. It is the very last option that is considered when a child is in advanced or end stage heart failure. A pediatric heart transplant, on average, will last 10-14 years before another transplant will be required.
The thought of a heart transplant used to overwhelm and terrify me. I will never forget the conversation we had with Lily’s cardiologist outside of her hospital room, on my husband’s 38th birthday, when we were told the news that there was nothing else that could be done to help our sweet girl. Our home hospital did not feel that Lily Grace was a good candidate for a heart transplant due to her unique anatomy, and she would then be rejected by two more heart transplant centers after this. Suddenly, the very thought that scared us to death become our heart’s cry. Please, somebody, give our daughter a chance at Hope!
Now that we are seven months post heart transplant, I am here to encourage you to not be frightened by intimidating words like “heart failure”, “terminal”, or “heart transplant”. While the journey to a new heart and the life long pursuit to preserve it are not simple, the reward of watching your child get the opportunity to live their life to its fullest is worth every sacrifice you will make along the way.
Transplant Evaluation
The process of your child being evaluated for transplant may be arduous and emotionally taxing, while at the same time a period of great hope. There is a serious shortage of donor organs, which means that donor hearts are considered a very precious resource and transplant centers are very selective in which children they will accept as potential recipients.
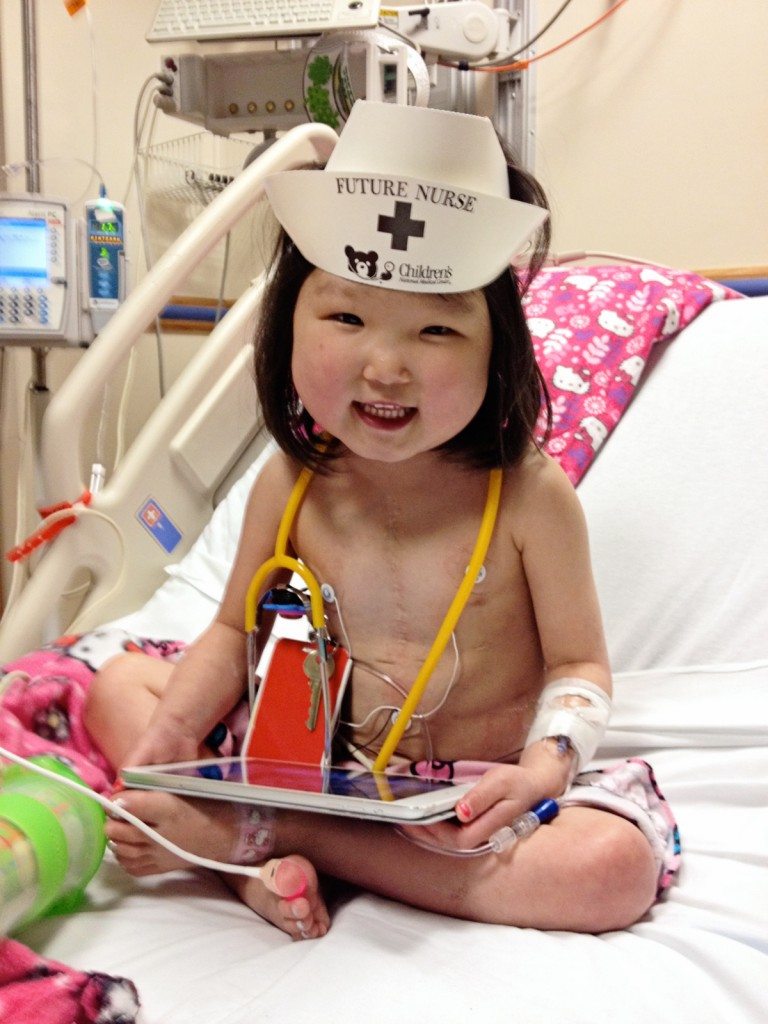

During the transplant evaluation process, your child meets with specialists from a variety of fields. These specialists may include Transplant Cardiologists, Transplant Coordinators, Cardiac Surgeons, Anesthesiologists, Social Workers, Neurologists, Dieticians, Psychologists, and Infectious Disease Specialists.
As part of evaluating the suitability of a child for transplant, many tests will be conducted including, but not limited to, blood tests (panel of reactive antibodies; virology testing for numerous illnesses such as Varicella, HIV, Cytomegaly virus, Epstein–Barr; and chemistry testing to check the health of the child’s other organ systems such as the thyroid, liver, kidney). Heart specific testing that may take place include echocardiogram, electrocardiogram, chest x-ray, cardiac catheterization, CT scan, cardiac MRI, abdominal and/or cranial ultrasound, and muscle biopsy.
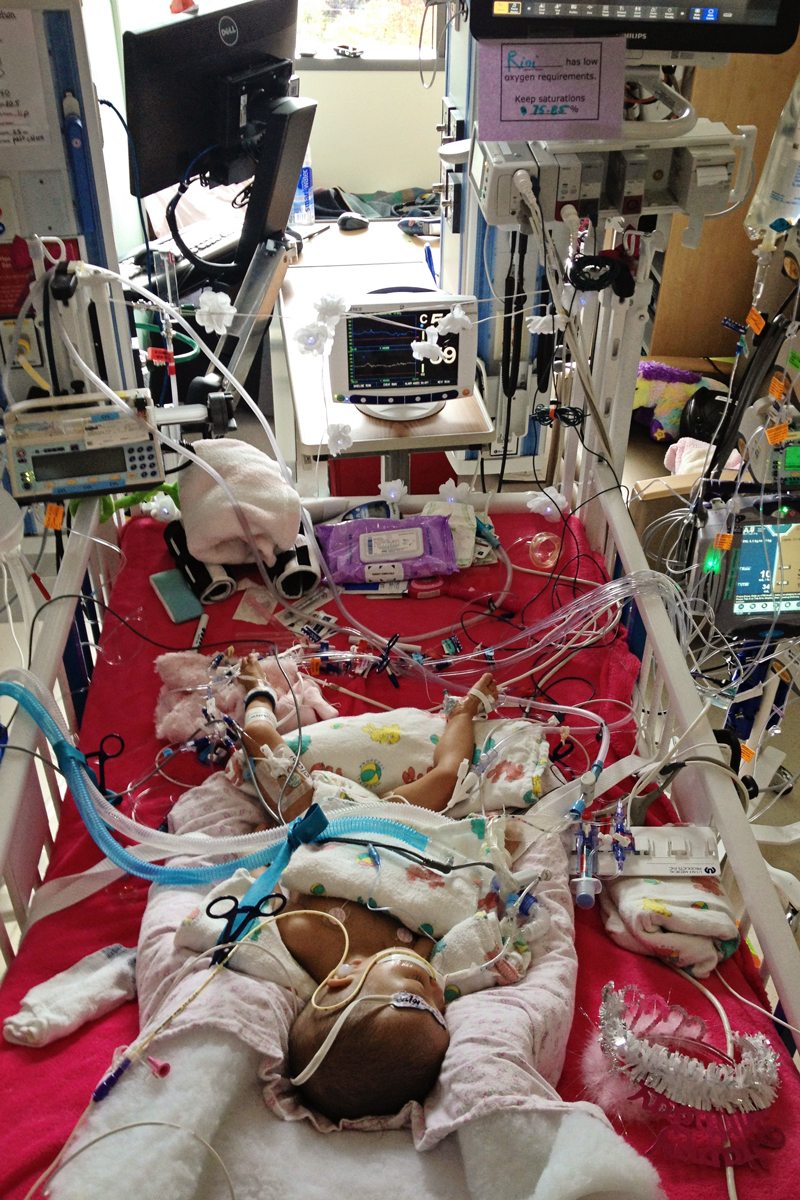
Families also meet with social workers to discuss insurance coverage, the ability of the family to meet the financial responsibilities of post- transplant care, and also the family’s ability and willingness to accept the challenges inherent in post-transplant life. Not all families choose to proceed with transplant, and not all families are found to be willing or able to comply with the instructions necessary to keep a post-transplant child healthy or to have an adequate psychological and/or financial support system.
After the evaluation is complete, which may take up to two weeks, the data will be presented at a transplant committee meeting and a decision will be made whether to list the child for transplant or not. This decision is based on myriad factors, and may be unique from center to center.
Not all children’s hospitals have heart failure/transplant programs, so families may need to travel out of state to a transplant center and may be limited by insurance coverage as to which transplant centers they may choose from. Transplant centers usually require that the patient reside no further than a two hour drive from the transplant center which may result in the need for a family to relocate. After transplant and discharge from the hospital, the child is usually required to remain within close proximity to the transplant center for up to several months during the critical post-transplant period.
Listing
If the committee decides to list a child for transplant, criteria dictates the child’s listing status. UNOS (United Network for Organ Sharing) is the national organization that oversees all transplant centers. The child’s information is input into the UNOS system, which ultimately matches donor organs and recipients based upon size, blood type, size of organ, accrued wait time, medical urgency, and other factors.
Listing Status: UNOS defines listing status and centers must follow the strict criteria. Appeals may be presented to the UNOS committee.
— Status 1A — This is the most critical status. It usually includes patients in the intensive care unit, on life support and/or high-dose intravenous (IV) medications to support their heart function. They may also have a ventricular assist device (VAD) or extracorporeal membrane oxygenation (ECMO) to support their heart function. The national average wait time for a donor heart at Status 1A is currently 3-5 months.
— Status 1B — Although these patients may be at home, they have advanced heart failure or other issues that warrant a higher status. The national average wait time for a donor heart at Status 1B is usually one year or more.
— Status 2 — These patients do not meet the criteria for Status 1A or 1B. Often, these patients are waiting at home for a donor heart and are taking oral heart failure medication. The wait time for a donor heart at Status 2 may be two years or more.
— Status 7 — This means that a patient is temporarily inactive on the heart transplant waiting list. This might include patients who have an active infection and cannot undergo transplant surgery until the infection has resolved, patients who are temporarily outside of the two hour distance from the center, or patients whose insurance has changed and need a new authorization or have lost insurance coverage.
Receipt of a Donor Heart
“While our daughter lay on ECMO life support after her second cardiac arrest, we prayed for God to strengthen our arms and shoulders so that we could bear the burden, carry our daughter, and help us to hold fast to the knowledge that ultimately we would be stronger for whatever lay ahead.” – Andrea
“Three days before we received the call that they had a heart for Lily, she and I had THE transplant talk where I told her how she would come to have a new heart. Immediately following our conversation, Lily prayed for her donor’s family knowing that they would be very sad when their child would die. There is no doubt in my mind that God was preparing our family for the arduous journey that was around the corner.” – Emily

When your child’s life depends on the receipt of a donor heart, it is a highly complex and emotional time. The pain of knowing that it will take another child’s death to provide hope and life to your own child can be difficult to process. Organ donation represents a raw yet beautiful process: that of redemption from darkness, of hope from despair.
When a donor heart becomes available, the donor’s information is input into the UNOS system, and a match is made. The potential recipient’s transplant coordinator is notified, and after consulting with the transplant surgeons, a decision is made whether to accept the heart or not. Reasons to not accept the heart may be because the heart is located too far away (causing the ischemic time to be outside of acceptable range), the donor heart’s function is poor, or the potential recipient is currently ill.
If the donor heart is accepted, out patient children will be brought to the hospital and preparations will begin for surgery. A transplant surgeon and nurse will travel to the donor’s hospital where the surgery to obtain the heart will be performed. Sometimes, the decision is made at that late stage to not accept the heart.
From Emily:
After being denied for listing at three transplant centers, our home hospital decided to list Lily Grace. Lily had been inpatient for three and a half months at this point battling uncontrolled Protein Losing Enteropathy (PLE) that caused her to become extremely puffy as well as her lungs to fill with fluid. My husband and I finally requested that hospice get involved so that we could bring Lily home to die.
As soon as the hospice team left Lily’s room, the heart failure cardiologist appeared at the door to tell us that she would like to present Lily to the transplant board again for reconsideration. Within 24 hours Lily was placed on the list as a status 1A. Lily remained a status 1A for six weeks until it was determined that her hospital discharge lowered her priority to a status 1B. Lily waited another six weeks at status 1B when we received the surprising news that they had a heart for Lily.
Lily’s transplant surgery took twelve hours, and we were told that she is the most complicated heart transplant to have ever been done in the USA. Lily’s new heart was connected to only her left lung since her right pulmonary artery clotted off after her fourth open-heart surgery rendering it discontinuous from her heart. Lily’s recovery was brutal, and she coded on multiple occasions due to seizures. She spent three months in the Cardiac Intensive Care Unit, and another three weeks in the step down unit before discharge. Lily has now been home for three months, and against all odds is absolutely thriving!
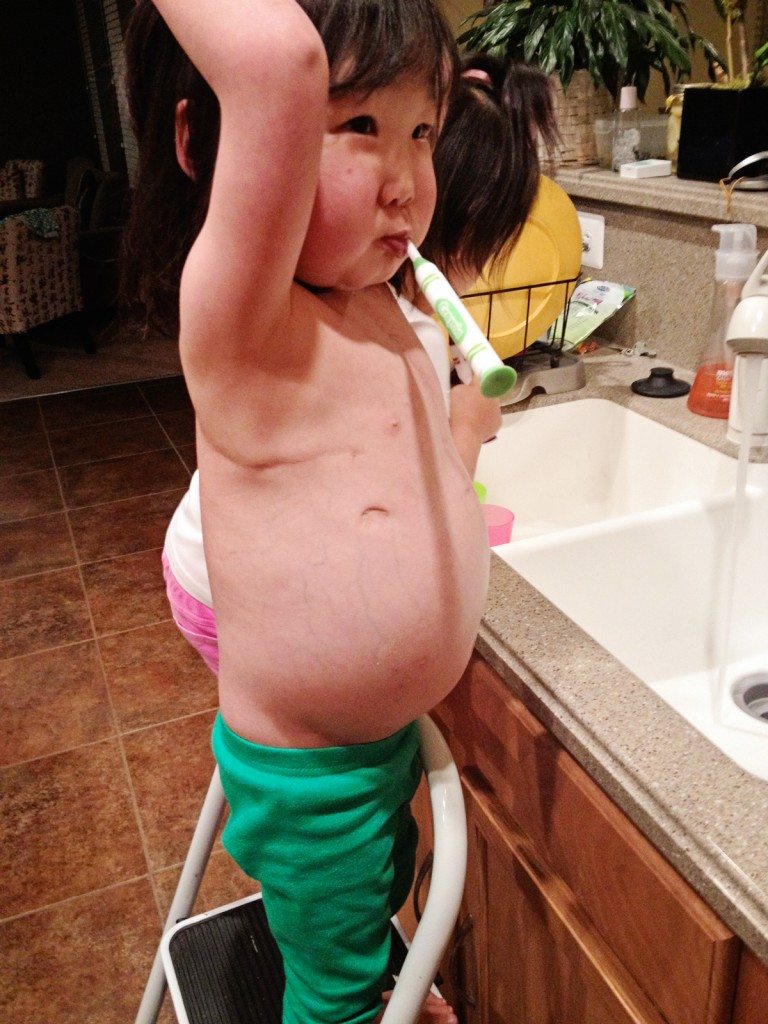
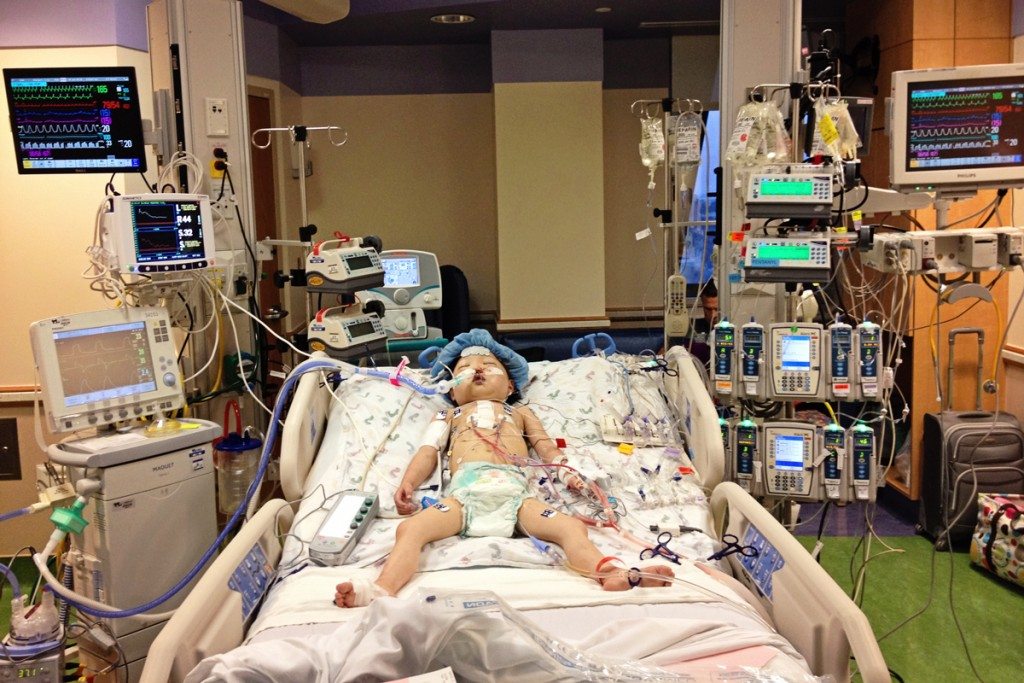
From Andrea:
Rini was highly critical, on ECMO life support after suffering two cardiac arrests, and listed at Status 1A. Children are only able to survive on ECMO for 2-4 weeks at most. But miraculously, she received a heart after only 19 days on the waiting list and 10 days after being placed on ECMO.
Her heart came from over two thousand miles away with a significantly longer than desired ischemic time, but was accepted due to her critical status. Her surgery lasted over twelve hours, and she came out on ECMO as her new heart was not functioning well enough to support her, although she was able to come off of ECMO several days later.
Her recovery was difficult, including another cardiac arrest, prolonged respiratory difficulties resulting in multiple intubation/extubation cycles, and several emergency surgeries. She remained in the Cardiac ICU for an additional three months post-transplant, and was finally discharged from the hospital after a total in-patient time of six months. Her first five months home were challenging, including multiple re-hospitalizations, but she is now thriving, blooming, and enjoying life!
*note* Rini and Lily’s recoveries represent the extreme end of the spectrum. Some children spend as little as two weeks in the hospital post-transplant.
If you are pursuing or parenting an adopted child with complex heart issues and have a question regarding cardiac care, feel free to email Andrea here or Emily here.


























Leave a Reply