We received our referral after waiting two years. The wait was grueling. In my online groups, people continuously posted that the wait for minor needs boys was so short. Not for us.
We chose minor needs for many reasons, but mostly because we have lived through two of our children being very ill in the hospital and eventually passing away. We didn’t want to go through this with another child so we chose as minor needs as we could. Also our 10 year old has had numerous surgeries which has been very hard on her and us, so our agency did not include needs that required surgery.
We received a referral for a 12 month old, whose needs included a self-healed heart condition (PFO) and a developmental delay. He was everything we’d waited for, and we loved him instantly.
Two months later we were handed a frail very sick 14 pound baby boy. He looked pregnant as his abdomen was very distended, and he had a 103.9 fever. We made it home and saw our international adoption doctor immediately. We told her about the fever and antibiotics our guide had given us. She felt a mass in his stomach. We needed an abdominal/renal/pelvic ultrasound – immediately, which meant we had to withhold fluids – including formula. The tech told us to go to the waiting room, but reminded us not to feed him in case he needed more testing. This was our first indication something was wrong. Finally the doctor told us our son had a massive fluid filled sac where his kidney was supposed to be. She had already made an appointment with the head of urology. That should have been another indication that things were bad.
Later at home – like most parents – we googled “fluid and kidney” and that is when hydronephrosis entered our lives. We researched it and of course had a list of questions. At first we were angry that China did not disclose this to us. We waited days on end for a referral, and I cried some nights thinking we would never get one. We finally get our referral, fall completely in love with our son, bring him home, and find out that the “minor” special needs are not so “minor” after all! So what do you do? You get over it. Put on your boxing gloves and get ready to the fight for your child! And, you thank God every second that this child was given to you.
His kidney was so massively full of fluid there was virtually no actual kidney material viewed on the ultrasound. His kidney was visible as a large lump on his abdomen.

We saw the urologist. He was quick with our appointment and assumed we had been told what was going on before we had arrived. I left in a daze. I quickly came home and joined all the hydronephrosis groups I could. I ask questions and received information that maybe I didn’t want, but got anyhow. I learned that hydronephrosis is congenital – meaning here in the United States it is usually diagnosed before birth, but in China with the lack of ultrasounds, it is usually diagnosed after birth.
Our urologist said his kidney has been this large since birth and all the damage that was done to it could not be reversed. Hydronephrosis can be unilateral or bilateral. It is graded based on of how much fluid is in the kidney or how dilated the kidney is. There are 4 grades (or 5, depending on who you ask): grade 1 is the most mild and grade 4 is the most severe. Grade 4 is where the kidney is dilated and the renal pelvis is also dilated, but the kidney contains some features of a kidney. Our son’s was considered more severe than that because there was no distinguishable kidney features, or “meat” as our doctor termed it. My thoughts on this were if there is no kidney and if whatever is in there is causing him to get infections (fever in China and at home), then take it out. If it is not serving a purpose and causing him pain and risking his life…. take the thing out. But the urologist said there was possibly still function in there. This is where my “gloves” came out. Prove it to me. Show me it is still working, and I will let it stay in there.
I shared my feelings with our pediatrician; he called the urologist, who made time to call me and talk. After our conversation, our son was scheduled for a MAG 3 with Lasix renal scan to assess function. This was very traumatic for him. It involved an IV, a catheter and being strapped down for three hours.
This test uses dye that the kidneys uptake and then takes images every second as the dye is peed out. The Lasix is given halfway through so urine is made and excreted faster. His test results indicated that he had 30% function in that kidney. Our doctor said that was a gross overestimation, he estimated only about 20% to 25% function in our son’s bad kidney. Each kidney in a normal body gives 50%. If one kidney is bad and gives 30% the other gives 70%, 60/40, 80/20 etc.. anything less than 15% is considered no function. If one kidney gives 30% and the other gives 30%, both kidneys are failing. However, if one kidney is good it will compensate for the other. This is why people can live with only one kidney. If one kidney fails, the other takes over that percentage in function. So our son’s kidney has 25% function and is failing. It will never regain any more function, and can worsen over time. His good kidney is compensating and functioning at 75%…..anything above 50% being normal.
We agreed to go ahead with the surgery as scheduled. Surgery included a pyeloplasty, which involves removing an obstruction at the ureteropelvic junction (UPJ). This obstruction is what causes hydronephrosis. The urine is unable to drain and backs up into the kidney stretching it out. Surgery also included a cystoscopy to place a stent, and drain the kidney. Our son’s surgery was done using a robotic device and involved three incisions. One near his sternum, on in his belly button and one in his pelvic region.
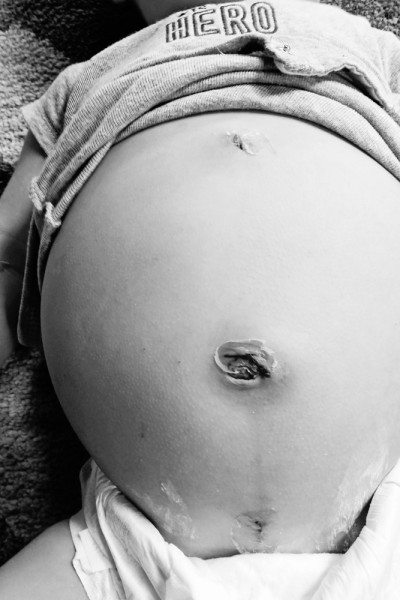
The surgery took five hours. Our son’s incisions looked huge even though they were only a half an inch in length. He had bladder spasms after surgery and didn’t do well with the pain meds and as a result, we had a two day hospital stay.
So what does the future hold?
Our son will have surgery to remove the stent, and then we will follow up with urology to see if the surgery worked. Our boy can live an unrestricted life. He will need to wear a guard over his kidney if he plays contact sports but other than that? No other restrictions will be necessary. There is a possibility the surgery did not work, and if that is the case, he will need more surgeries. There is a likelihood he could lose this kidney…. there is also a chance that his other kidney at some point could go bad. Although we have been assured that this is rare.
For now we are just going to hang out and enjoy every second with our son.

Kidney Facebook groups (all groups are closed):
Parents of Children with Hydronephrosis
China Kidney Kids
Hydronephrosis in Children
Web Information:
Kidney.org
ChildrensHospital.org
– guest post by Amy

























Leave a Reply