My son, J, has Larsen syndrome, a condition of multiple joint malformations. I write this in hopes that it shows how manageable this condition is.
In the summer of 2012, I saw a video that an advocate had posted, of a little boy riding a scooter around a play area. His nanny was directing him to go to the play set, and climb up, then slide down. She then had him go to some chairs, climb up, remove his jacket, and recite a song. The boy was so agile, so confident, and maybe even a little bit cocky? It was in his every gesture and movement, “Is this it? This is all you needed? Easy-peasy-lemon-squeezy!”
I was a goner.
The boy in the video had one leg that bent the wrong way. The left leg bent out in front of him, instead of to the back. He got around exclusively on his knees. His feet appeared to be clubbed, and his arms were held at 90 degree angles. He appeared to have a pigeon chest. It didn’t slow him down one iota.
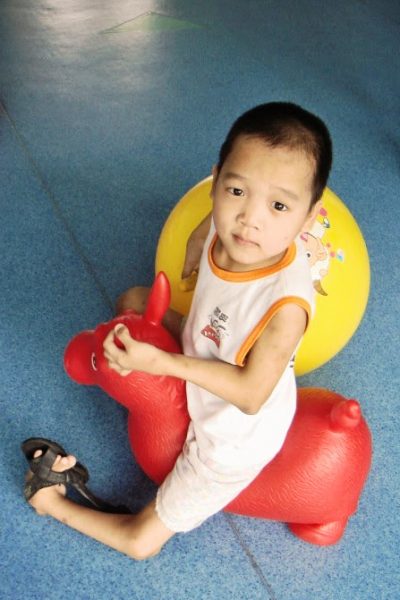
The definition of Larsen syndrome, according to the U.S. National Library of Medicine is “…a disorder that affects the development of bones throughout the body. The signs and symptoms of Larsen syndrome vary widely even within the same family. Affected individuals are usually born with inward- and upward-turning feet (clubfeet) and dislocations of the hips, knees, and elbows.” (source)
I showed my husband the video, and we called our agency. J had been on the waiting child list for almost 4 years. We requested J’s file, which had very little in it, other than mentioning a couple of his obvious issues. I sent the file to be reviewed by a doctor, and she was as bowled over as I was by his video. This doctor didn’t hold out much hope of correcting any of his issues, but she was wildly supportive of his ability to have an active and productive life. We locked his file.
We requested updates, and received x-rays and more photos. I sent them to a local orthopedic surgeon, and to an international adoption clinic, mainly because I am an information junky. Our local surgeon wasn’t very optimistic or helpful. The IAC doctor was wonderful, but cautioned us that the pigeon chest appeared to affect his lungs, and she suspected Spina Bifida. She wanted us to be prepared.
Eight months later, on my husband’s birthday, we met our son. He sang his new daddy “Happy Birthday” in Mandarin. He was almost 8 years old.

Upon arriving home, we started the rounds of doctor appointments that you do when you bring home a child with unknown medical history. I am listing them with their outcomes in the hopes that it will highlight some of the possibles with Larsen syndrome, as well as what it doesn’t necessarily mean.
We went to the IAC, where they did blood work and sent us home with the infamous stool sample kit. They referred us to a spine doctor as well as a more general orthopedic doctor, who first told us J had Larsen syndrome. This appointment was where we found out the nature of all J’s joints that are affected. The orthopedic doctor confirmed a dislocated hip. He also clarified hyper-flexible shoulders and fingers, with extreme ranges of motion, as well as elbows that range from zero to 90 degrees, but can’t go further. His wrists have a limited range of motion, as well as his thumbs.
His feet were both turned completely over, with the left one being located on the side of his ankle, instead of at the end of it. His knees, as mentioned initially, were severely affected. One bent forward, with range of motion in two planes (he could touch his toes to his nose, as well as lay his left foot on his right shoulder), and the other bent back and to the left, with a range of motion of zero to 90 degrees.

After examining the hip, the decision was made to do nothing about it. We are fortunate in that it causes him no pain, and it was left untreated so long, they felt the likelihood of a successful surgery was slim. It would, in all likelihood, dislocate again. The potential for more harm was greater than the potential for gain. We had this opinion seconded by another orthopedic specialist.
J’s shoulders and fingers are never an issue, and his thumbs only rarely so far. He uses a pencil grip, like you can find at T@rget in the school supply section, to allow for a firmer grip on his pencil, and that’s it. His wrists seem only to hamper him when he tries to “rev” a motorized scooter, like you would “rev” a motorcycle, with the hand grip. (I admit that having a motorcycle not be a viable mode of transportation for him causes me relief.)
We inquired about attempting to correct J’s elbows because J wants to perfect his three-pointer, and feels his elbows are hampering his long-term prospects as a ball player. The ortho doctors feel trying to do anything about his elbows would be ill-advised. He can perform all self-care, as well as school work, with his elbows as they are. It would be foolish to risk losing any range of motion, if the surgery was unsuccessful, in an effort to gain a better basketball shot. (J disagrees with this opinion, and still questions the decision.)

We initially hoped that something could be done about J’s knees and feet that would allow J to walk upright on his own legs. He really wanted to be taller. However, on X-ray and MRI, his knees just weren’t put together like a knee should be. His feet were also going to be a problem, being so severely affected and left unattended for so long.
The options we were presented with were a) to apply external fixators to try and turn his feet, have multiple surgeries, wear leg braces, and use crutches for life, accompanied by chronic pain, b) leave him to get around on his knees, until his knees gave out, at which point he would be in a wheelchair, which amounted to continuing to get along as he had been for 8 years, or c) amputation and prosthetics. After numerous opinions, research, and prayer, we opted for amputations and prosthetics. The surgery was done one year after he came home.

The spine doctor we saw said J does not have spina bifida, nor does he have scoliosis, which our pediatrician suspected. Multiple vertebrae are formed oddly, due to the Larsen syndrome, and combined with his dislocated hip, it causes his spine to appear suspect on x-ray. We still get conflicting reports from other doctors regarding the presence or absence of scoliosis, but the spine doctor J sees is one of the best in the country, so we choose to follow his plan of care. The amputations actually improved the appearance of J’s spine, due to now having a more normal gait.
Of note, a person with LS can have kyphosis, which is a curving of the spine that causes a bowing or rounding of the back, which leads to a hunchback or slouching posture, according to the U.S. National Library of Medicine. This can lead to some special issues of its own, which I know next to nothing about, since in J’s case, he has lordosis, which is the opposite. This has caused no major problems, although leaning forward to write for long periods, or lying flat on his back, such as at the dentist, are uncomfortable. A pillow or even his arms folded under him, help him to be comfortable at the dentist.

During the physical needed to leave China, they told us J was blind in his right eye. After arriving home, the opthamologist here tested him and he actually has 20/20 vision.
We also had a hearing test done, where it was discovered he has moderate hearing loss in both ears. Hearing issues can be a component of LS, due to malformations of the bones in the ear. In J’s case, his ears appear to be formed normally. His hearing loss is sensori-neural, instead of structural. He began wearing hearing aids, and receives speech therapy weekly.

Due to the pigeon chest, and what appeared like a concave rib cage on one side, the pediatrician referred us to a pulmonologist. I was pretty confident there was nothing wrong with J’s lungs. He held his breath in the bathtub in Guangzhou for 20 seconds, “swimming”, right out of the gate. The pulmonologist’s findings confirmed this, but he referred us to a cardiologist, “just to be safe”. The cardiologist found a benign murmur, something “one in ten people on the street have”, and cleared him. J receives no treatment for the murmur, and we don’t have to follow up with the cardiologist.
It was suggested around this time that we have J evaluated by a nephrologist, as well, due to his hearing loss. The ears develop en utero at the same time as the kidneys, so even though his hearing impairment is not due to any physical malformation that anyone could find, they thought having his kidneys checked would be prudent. There were no issues with his kidneys.
So, here we are, three years later. J remains ridiculously healthy. He has had two ear infections, in three years, and those were right after coming home. He hasn’t had so much as a bad cold, otherwise.
He continues with his speech therapy, which will probably continue for the long term. He will need new hearing aids approximately every three years. He goes to physical therapy off and on, as he grows, or when he gets a new pair of prosthetic legs. Typically children outgrow prosthetics every 18 months to 2 years. J is off that pace by a bit…. he needed new ones about 14 months into his first pair! I would suggest researching hearing impairment as well as limb differences for more information on these topics.

J is unbelievably agile, strong and coordinated. When he received his first pair of prosthetics, he was scheduled to have a week of twice-daily PT, to learn the basics of getting around, up and down. The first task they set for him, getting down off a bench onto the floor, he mastered in about seconds. He never looked back. I saw that same look on his face, the whole week, that I had seen in the initial video. “Is that it? That’s easy-peasy-lemon-squeezy!”
The surgeon, the physical therapists, and the prosthetists had never seen anyone handle the surgery, recovery, and prosthetics like J. To this day, his prosthetist just shakes his head and says, “People just don’t get a new pair of legs, and take off on them like that. It supposed to take time. It supposed to take practice. HE is amazing!”
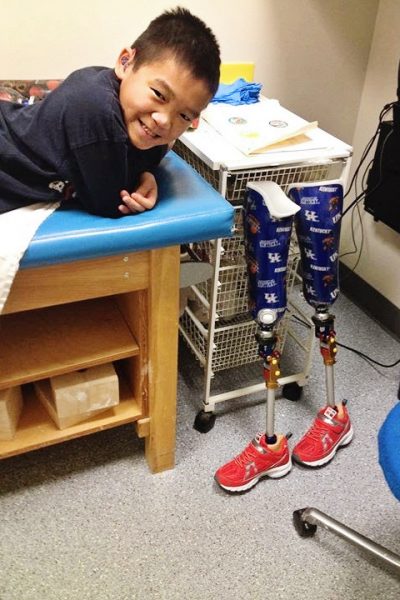
In conclusion, each individual case of Larsen syndrome can look very different from the next, but the common thread I have seen in the few cases I have seen and read about, all in children adopted from China, is a tremendous resiliency and strength, both of body and character, that truly allows them to live very active lives, with very little accommodation.
– guest post by Elizabeth

























Wow! This kid is amazing!! If he continues to be interested in wheelchair basketball, check out camps (& maybe college) at UW-Whitewater (WI)!