Rini, our youngest of six children, was adopted in August of 2013 at end stage heart failure stemming from complex, single ventricle congenital heart disease. She was admitted to the hospital immediately upon arrival home and within two weeks it was determined that she was inoperable, her only hope would come through cardiac transplant. She was initially found to be ineligible, but that would change thanks to a heart failure/transplant program that chose to take a chance on hope and optimism.
Much as we owe her life to the sacrifice made by her birth family in letting her go, we also owe it to the incredible, selfless act of organ donation made by a family in the midst of the incomprehensible loss of their child.
This series is a retrospective of the weeks leading up to Rini’s transplant which took place on November 13, 2013, and it is my hope that it will help to bring awareness to the importance of registering to be an organ and tissue donor.
We all have the power to be someone else’s miracle.
Donate Life!

From September 29, 2016:
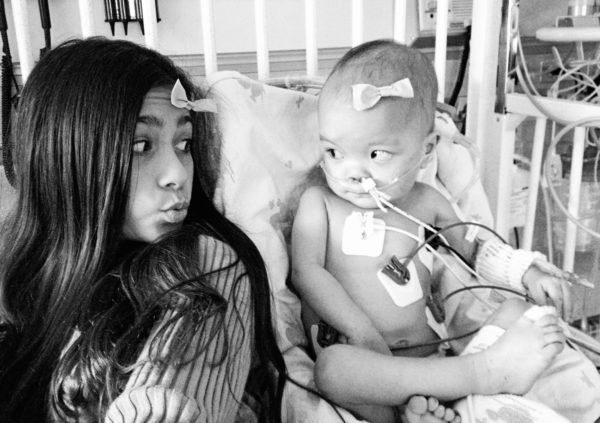
On this day three years ago, I went out into the hall and introduced myself to a young woman who would walk by Rini’s room every day. I learned she was 22 years of age and visiting her 13 year-old sister who was in the room just down the hall from us. Her sister was dying of a brain tumor.
Each day when she would walk by Rini’s room, she would hesitate a bit. I got the feeling that she wanted to meet my sweet little one who would point, wave, and blow kisses to her as she came down the hall. So I invited her in, we talked, and she was able to enjoy a brief respite from the bedside vigil she kept in her younger sister’s room.
This young woman came to visit Rini every day from then on, and sometimes her entire family would gather around the entrance to Rini’s room to delight, smile, and laugh at Rini’s cute antics. Then came the day that they didn’t come by, and we never saw them again.
When your child is dying and in the hospital, surrounded by other children whose time on this Earth is limited, you ponder many things. Children die, and far more of them than most people realize. My acceptance of the platitudes uttered during times of strife was stripped away during this process. As my friend, Lisa Ellsbury wrote in a comment to my September 23rd post, children don’t die because enough prayers aren’t said, and children don’t live because somehow they are “winners”. We live in a broken world. Disease exists. Bodies fail. What I did believe before Rini, and even more strongly during her critical time and since, is that as God grieves with us during times of tragedy, and we can try and find a way to use our pain for good. He is there to carry us during our darkest times.
From September 29, 2016:
On this day three years ago, we let go of a dream. It wasn’t a bitter surrender, but rather a decision made out of hope. It was on this day that we made a decision that ran contrary to what many physicians caring for Rini were hoping to achieve.
On this day, we chose to release the goal of Rini coming home.
For the past week and a half, we had been trying to find a method of respiratory support that would allow her to be home while we waited, hoped, and prayed for a transplant center to welcome her for evaluation. High flow room air yielded the best result, short of placing her on a ventilator. With each alternative that we had tried, she had gone back into respiratory distress after 36-48 hours.
The day before, we had attempted CPAP which was a complete disaster. She was hysterical and we scrapped it after just a few minutes. The whole point was to provide her comfort, not to send her heart rate soaring and her 02 sats dropping, and deny her the ability to comfort herself with thumb sucking. The smaller version of CPAP, where it’s not a full mask but rather one that just covers the child’s nose, was not an option because of Rini’s NG tube.
From my journal – September 30, 2013:
“This morning, I found myself weary and, frankly, getting irritated with what was beginning to feel like a never ending ride on a carousel that we were subjecting Rini to. I spent the day reflecting on all we had tried, and I spoke several times with Eric. I asked the cardiology team that was rounding to call our cardiologist and have her come and see me. When she arrived after clinic this afternoon, I asked her how she felt about the current plan. She told me exactly what she thought, and lo and behold, it was right in line with what Eric and I were beginning to feel.
The only chance that Rini has is transplant, and the only way that she has a chance to get to the point where she can be fully evaluated is if she is nutritionally stable and gains weight. While she was at home for those 9 days, she gained no weight and actually lost just a bit despite enteral feeding 22 hours per day supplemented with some oral feeds. We brought her home from the hospital earlier in the month in order to give her the psychological benefit of being home, but what we have come to realize is that home may not be the best place right now for her physical body. At home, she was agitated often because mom and dad could not be with her constantly, she found it difficult to rest for any substantial length of time because of all of the distractions: a cat would walk by and catch her attention, she’d see a sibling outside the window and yell to go outside, she would understandably want to be wherever the action was in the house so she would want to be moved from place to place dozens of times per day. And as the days went by, her coloring grew worse, her breathing became more labored, and eventually she began to go into respiratory failure which landed her back in the hospital. And with all of that expenditure of energy came a lack of weight gain and more stress on her heart.
Eric and I recognize that by bringing her home on respiratory support that is not sufficient (high flow is not available for in-home use), we will be engaging in a cycle. She would most likely end up needing to be readmitted within a week at most, judging by how she has been responding to non-high flow respiratory support over the past 10 days here.
The other option would be not to re-admit her. But that, we know in our hearts, is not an option. She is not ready to go, and we are not ready to let her go. We cannot make that decision while her body is in the state that it is in. She hasn’t had a fair shake of it yet.
This plan will also provide stability to our kids at home, rather than the day-to-day uncertainty as to when I am coming home. I will stay until Friday night, and then Eric will take over for a week, and then we will switch. Rather than looking at Rini’s progress in terms of day to day, our cardiologist wants us to view it a bit further out like week to week.
Now the stress of trying to find some new way to get her home is lifted, since we have accepted that bringing her home is probably not the best way for her to get to where she needs to be. It was a bit of a bitter pill to swallow, but once we recognized what was occurring and we accepted what was truly best for her rather than what we hoped would happen, we all felt a huge sense of relief.
We don’t know how long this will take, and we don’t know whether her heart failure will progress faster than her overall stability. By the assessment of all involved in her care when we first arrived at the hospital from the airport on August 30, she was probably within a month of death, so we are all attempting to bring her back from that place.
Keeping her here may be the best we can do to give her a fighting chance at making it to transplant evaluation.
I spoke at length with our cardiologist about disease progression, and what it looks like in this type of situation. My biggest question was whether we can halt the progression of her cardiac disease, and the answer is “no”. Any intervention we attempt may serve to slow the progression, but it won’t stop it. She walked me through the steps, the respiratory interventions, the drugs, and what happens to the body as heart disease continues. This helped me to be able to gather my thoughts and have a talk with Eric so that we can at least be aware of what we will be faced with and how we can assist Rini if she does not receive transplant in a timely manner.
So we have chosen to keep her as calm and supported as possible while we strive towards that goal. Once she is there, her cardiac function will be reassessed. Our biggest hope is that by some miracle her ventricular function will show remarkable improvement to the point that maybe, just maybe, her valves can be repaired as the first of many surgeries she will require. But if that does not come to fruition, than at least the transplant centers may do a full evaluation and make the decision as to whether she will be a candidate.
So between now and then, we will take it one step at a time and continue to love our little girl. Our Empress Rini has a blue chair next to her crib, and every day when I am up and about in the room, she yells, “Mama!” and points to the chair. I sit, and she rolls over on her right side and dangles her little legs out between the slats of her crib and stares at me. I joke that I am her lady-in-waiting, there to serve her. We spend hours next to each other, as she holds my hand or we play peek-a-boo and other games together. And every day she becomes more engaging and delightful.”

From October 1, 2016
Three years ago today, we had accepted that Rini would remain hospitalized. I felt at peace, but only for a short while. Soon an underlying current of sadness presented itself. This awful roller coaster of highs and lows, of hope mixed with resignation and acceptance, was only just beginning. Nothing could have prepared me for what was to come.
In only one week, Rini would leave this place of relative stability and begin her rapid descent into the end of end stage heart disease. Somewhere inside of me, I knew it was coming. I began preparing for it. Over the next week, we would have many visitors, and I wonder if those who love us sensed it, too. Eric felt it as well, he tells me now. But during that time, we just couldn’t give voice to it to one another quite yet.
From October 2, 2016
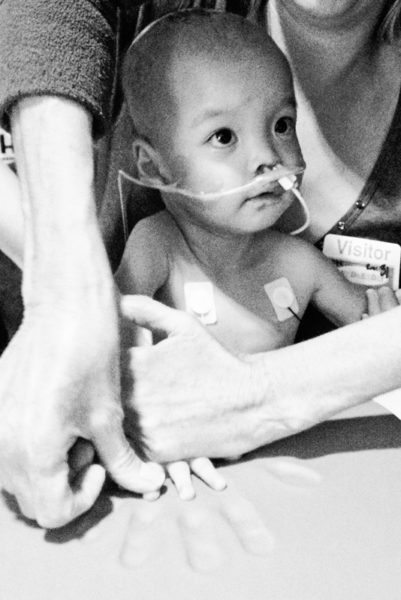
On this day three years ago my steadfast friend and fellow heart mom, Beth Anderson, came to the hospital to preserve a memory. I could say that I wanted to capture Rini’s precious handprints and footprints in much the same way I’ve done for each of my other children, such as keeping a lock of baby hair or their first walking shoes.
But the truth is, while we were keeping our eyes fixed on the goal of a successful transplant, we were simultaneously preparing to lose her.
I remember the confusion and guilt of that time. Was I betraying her by trying to brace myself for her death? Was I losing hope and giving up? I recall feeling as riled when friends and acquaintances assured me of her survival as when they offered their condolences regarding her seemingly assured death. It was a terrible limbo.
I am a realist and a very pragmatic person, and also one who never for a single moment believed that somehow my family would be immune to the heartache experienced by far too many parents.
Through it all, we just yearned to honor and respect Rini. After all, she was the one who was fighting to survive.


























Leave a Reply