Rini, our youngest of six children, was adopted in August of 2013 at end stage heart failure stemming from complex, single ventricle congenital heart disease. She was admitted to the hospital immediately upon arrival home and within two weeks it was determined that she was inoperable, her only hope would come through cardiac transplant. She was initially found to be ineligible, but that would change thanks to a heart failure/transplant program that chose to take a chance on hope and optimism.
Much as we owe her life to the sacrifice made by her birth family in letting her go, we also owe it to the incredible, selfless act of organ donation made by a family in the midst of the incomprehensible loss of their child.
This series is a retrospective of the weeks leading up to Rini’s transplant which took place on November 13, 2013, and it is my hope that it will help to bring awareness to the importance of registering to be an organ and tissue donor.
We all have the power to be someone else’s miracle.
Donate Life!

From October 3, 2016:
On this day three years ago, I was preparing to head home to spend the next week with our other five children. Leaving Rini would be excruciatingly difficult, as would be leaving my other children in a week’s time. Along with anxiety, guilt would become a constant companion of mine over the weeks and months to come.
Through my work at Little Hearts Medical, I speak to many families, some who are reluctant to adopt a complex CHD child because they are worried that they won’t be able to meet the needs of all the individuals in the family during a child’s hospitalization.
If they ask me my advice, I give it. There is no way to sugarcoat it.
Everyone’s needs will not be met all of the time.
But as awful as that idea is to entertain, the unexpected result of that time can be individual and familial growth and a profoundly deeper appreciation for each other during times of togetherness. Of course, each individual family must determine whether they want to embrace that challenge. But for our family, God showed us so many precious gems that otherwise would never have been revealed to us were it not for the cracks and fissures that came to the surface during that arduous time.
The stress of those months brought out the worst in me and as a result, it brought out the best in me. It was another of God’s blessings and Rini’s Gifts.
From October 4th, 2016
Remember how yesterday I wrote that the stress of this time three years ago brought out the worst in me, but in doing so, it brought out the best? Well, here goes…
Three years ago on this day Eric came up to the hospital to switch places with me for a week. Leaving Rini was beyond difficult, and I felt like I was committing an egregious misdeed by leaving my baby who loved nothing more than to lay on her side in her crib, stare at me and hold my hand. But once the sliding glass doors of the hospital opened and I walked out into the cool October air, I inhaled deeply and began to look forward to my temporary respite from sadness in close quarters.
The thing is, I’m really good at being in the hospital with my kids. I enjoy medicine, nurses, doctors, and being a support and advocate for my kids. But what I was about to learn is that I was phenomenally deficient when it came to balancing my emotions during times of medical crisis. In other words, I did not allow for pain or for tears. I was about to learn that there would be a price to pay for that.
I walked in the door at around 10pm to a house that looked like a category 4 hurricane had swept through. I lost it. Oh yes, I lost it indeed. Neat and tidy is my equivalent to control, and in that house on that night, I had none. Suffice it to say, it wasn’t my finest moment as a parent or a spouse. My parents stepped in a few weeks later and hired a cleaning service to bring our home back to my ridiculous standards on the days in the future when I would return from my hospital shifts. There is no doubt how much they love their son-in-law to have protected him in such a way from my OCD-induced wrath.
I had a lot of amends to make once the dust of Rini’s critical time had settled.
From October 5, 2016:
On this day three years ago, I attempted to vindicate myself from the prior night’s meltdown by chilling out and watching my kids make a mess in the backyard. I still remember that day, and how cool and crisp it was with the sun shining so brightly.
Back at the hospital, Rini would spend what would turn out to be her last night of relative stability before she began her steep decline.
From October 6, 2016:
On this day three years ago, I was doing my best to make memories and soak up my time with Sophia, MeiLi, Tristan, Bryce and Scarlett against the backdrop of boundless anxiety and uncertainty. Meanwhile, Eric and Rini were enjoying their time together at the hospital, although it took Rini a couple of days before she would allow Eric to sit in “my” chair next to her crib!
Despite her sunny disposition, Rini was slipping back into respiratory distress and no longer benefitting from the support that she had been on for the previous two weeks. This was also the day that Rini’s washcloths first made their appearance. Her desire and later her insistence to have her body covered in damp, cold towels would become our gauge of her cardiac health. She also began to refuse to be covered in blankets or to wear any article of clothing, including socks.
Later, her heart failure team in Seattle told us that many children in late stage heart failure feel chronically hot, despite the fact that their bodies often feel cold to the touch due to poor blood perfusion. Rini’s hands and feet were like ice, and it was becoming difficult for her doctors and nurses to feel her peripheral pulses. She was also beginning to chronically vomit.
Soon, her kidneys would begin to struggle and her edema would return.
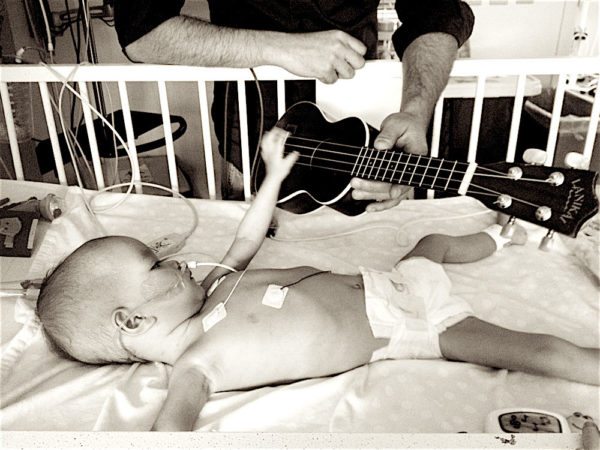
When we arrived home from China on August 29th, her local team did a beautiful job of slowing down the rapid decline in her health. Metabolically it was estimated that she was within four weeks of death. But despite the brief respite that support had granted her, ultimately there was no stopping her body from beginning to shut down. Her heart was too damaged and diseased.
The goal was to use the least amount of support possible for the longest amount of time, as we were engaged in a desperate numbers game. Every intervention has its consequences so in order to make sure that we didn’t use up our arsenal, nobody wanted to initiate any specific type of support before it was critically necessary. That is why she was placed on the intermediate care floor rather than the ICU when we readmitted her after her initial hospitalization and 9 days at home.
But it was beginning to look like bringing out the big guns would soon be necessary. It was a terrifying, gut-wrenching proposition. After all, she was still being denied transplant evaluation.
Our baby was beginning to run out of time.


























Leave a Reply