Rini, our youngest of six children, was adopted in August of 2013 at end stage heart failure stemming from complex, single ventricle congenital heart disease. She was admitted to the hospital immediately upon arrival home and within two weeks it was determined that she was inoperable, her only hope would come through cardiac transplant. She was initially found to be ineligible, but that would change thanks to a heart failure/transplant program that chose to take a chance on hope and optimism.
Much as we owe her life to the sacrifice made by her birth family in letting her go, we also owe it to the incredible, selfless act of organ donation made by a family in the midst of the incomprehensible loss of their child.
This series is a retrospective of the weeks leading up to Rini’s transplant which took place on November 13, 2013, and it is my hope that it will help to bring awareness to the importance of registering to be an organ and tissue donor.
We all have the power to be someone else’s miracle.
Donate Life!

From October 7, 2016:
On this day three years ago, Rini’s cardiology team approached the transplant centers again about her evaluation candidacy and was firmly told that the answer was still “no”.
This evening when I asked Eric how he felt on that day, his response was, “Desperate and scared.” That about sums it up.
Rini was in decline, her breathing had become increasingly labored, she was no longer tolerating her feeds and she could only endure sitting up for a few minutes. What looked like weight gain was actually edema. I still remember how after that day she would look at us and pat the bed behind her to let us know that she wanted to lie back down. Something in her eyes was changing, too.
In just four days, a conversation would take place that would ultimately change the course of Rini’s life, and bring our focus onto a hidden gem nestled in an emerald city four hours north of us.
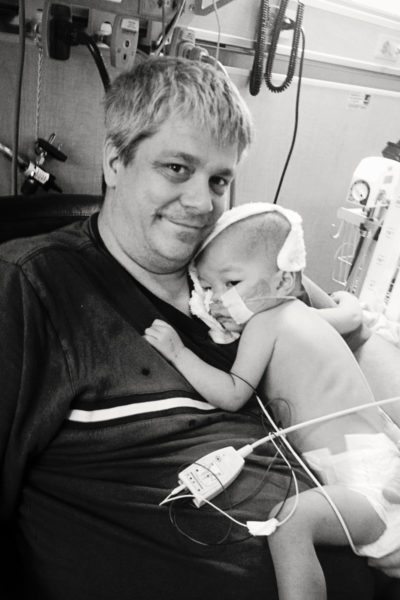
From October 8, 2016:
On this day three years ago, two of the world’s most supportive grandparents arrived in Portland from Los Angeles. I was still home with my little ducklings while Eric was loving on our baby girl at the hospital.
The last time my parents had seen Rini was the night we arrived at LAX from China. They had taken us to a hotel near the airport where we spent several anxious hours with our new daughter, trying to keep her hydrated with a medicine dropper while waiting for our early morning flight to PDX. Children’s Hospital Los Angeles had been notified by our Portland cardiology team and were ready to admit Rini if we felt she could not wait until we arrived home. Looking back at everything that transpired, I understand why our cardiologist said after looking at the labs drawn in the ICU where Rini was a patient in China, “If she is admitted in Los Angeles, she will not leave.”
Often I wonder what that outcome would have been. When you have a child whose only chance at life is if another family’s child dies, it calls many things into question, at least it did for me. I’ve never been one to believe that God picks and chooses which children live and which children die. I don’t believe that Rini survived because God has big plans for her on this earth anymore than I believe He therefore didn’t hold the same hopes for her donor. Rini’s donor wasn’t sacrificed so that my child could live. God has big plans for all of his children. God wants all children to be loved, to grow, thrive, and have productive lives.
Although I wouldn’t recognize it for another 35 days, something was being molded within me.
Rini’s journey to transplant was also my journey to my deeply personal understanding with God, to my reconciliation of sorts. I had grown up with an Old Testament view of the world. An eye for an eye. Yes, I believed in grace, but even though on an intellectual level I knew better, looking back I see that my safety mechanism was to tell myself that somehow I could inoculate myself against the wretched pain of this world by being a good person.
I think, to be honest, I was afraid of God and what He might do to me if I misbehaved in some way.
When you are the parent to a child whose future is so uncertain, and all around you there are other families suffering the most devastating loss in this world, the easy answers begin to ring hollow. I saw wonderful families of all walks of life… Christian, Muslim, Jewish, Atheist… all in the midst of the most difficult battles. Some children lived. Some children died. There was no outward rhyme or reason. The Type A person that I am desperately wanted to know why! Perhaps if I could figure that out, I would have some control over what my own child’s outcome would be.
It would take the next month, the most difficult month of my life to this point, to allow that need to be ripped down. I had to learn what faith was really about. And for me, it wasn’t about believing that everything would turn out in a way that protected my own heart.
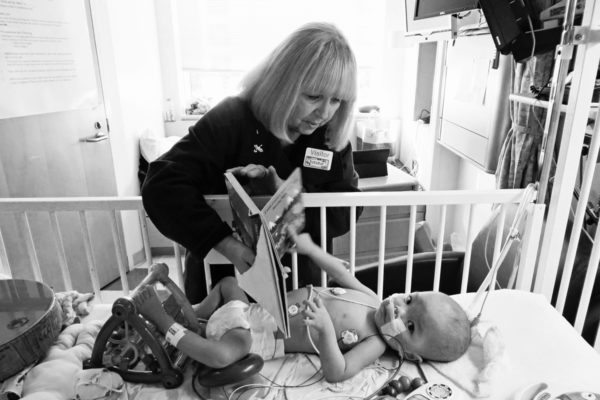
From October 9, 2016:
On this day three years ago, I dropped the kids off at my in-law’s and proceeded to spend several hours grocery shopping so that the house would be well stocked for Eric’s next shift at home which would begin in two days.
I know that many families who have children with ongoing medical needs can relate when I say that during critical times with your children, there can be a marked shift that takes place within your relationships. Some friends you’ve had for years mysteriously vanish. Other people who were on the periphery become steadfast supporters. And then there are the total strangers who you are convinced are angels in disguise.
Grieving and then accepting the loss of some friends was a process. I understand that not everyone feels equipped to support someone during times of great stress and sadness. They may feel awkward, impotent and unsure of what to say or do. In some cases, they may disagree with or even resent you for choosing a path in life fraught with challenges.
My advice to anyone who cares about someone who is going through a tumultuous time is this: say something kind – even if it’s just a text that states, “I just don’t know what to say, but I’m thinking of you.”
Don’t be afraid to bother your friend. Trust me. Silence is the worst, most intrusive sound.
Do not make specific offers of help or say, “Let me know if you need anything,” unless you truly mean it. First off, many people will not pick up the phone and take someone up on that while they are in the midst of crisis. Second, if they do they may find out very quickly that the other person never intended to follow through on the offer. That experience is awkward and painful to say the least. Taking it upon yourself to fortify your friend will always be appreciated.
But back to those angels in disguise. On this day three years ago, I was unloading my massive freight onto the belt at my favorite discount supermarket, which is the type where you are responsible for bagging your own groceries. Maybe there was something written on my face. Maybe it was my eyes, which always felt like they were brimming with tears during that time. Whatever it was, as I was emptying my cart onto the belt I looked over and saw that an older gentleman had started bagging my groceries for me. He looked at me and said, “I thought you might like some help today.” I just stood there and started to cry softly. After I had paid, I went over to him and thanked him, and told him how much his kindness meant to me. He just smiled sweetly.
It felt like God had given me a hug.
From October 10, 2016:
On this day three years ago, we had a glimmer of hope. The previous evening I received a call from Eric along with Rini’s cardiologist, Dr. Carlson. Rini’s labs were indicating that she was making gains in an area critical to her transplant evaluation eligibility: her prealbumin level.
The numbers below illustrate prealbumin ranges. You see how under 5.0 mg per dL is critically low? When Rini arrived home from China hers was 2.0 and as such, her body was literally eating itself. This is what led her physicians to surmise that she would have survived at most for another 4 weeks in China.
less than 5.0 mg per dL = Poor prognosis
5.0-10.9 = Significant risk; aggressive nutritional support indicated
11.0 to 15.0 = Increased risk; monitor status biweekly
15.0 to 35.0 = Normal
Malnutrition of this magnitude is a serious contraindication to transplant. A child can’t heal from such a major surgery if their body is not able to generate new tissue. One of the official “Exclusion Criteria” for cardiac transplant is the “Presence of non-cardiac disease that can substantially diminish the chance of success of the transplant or benefit gained after transplant”. Severe malnutrition is one such disease.
Her body’s inability to recover from physical insult was evident. Rini had been unable to heal from a burn she received in the Chinese ICU from a pulse ox being left on her toe for too long, and she had painful, weeping open wounds on the sensitive parts of her body that were caused by inconsistent diaper care in China.
Constant, specialized care over the past month and a half under the watchful eye of the Chronic Wound team had not been able to bring sustained healing. Her nurses and we were engaged in a never-ending cycle of applying ointments and barrier creams, for as soon as Rini eliminated her skin would break open like wet tissue paper.
The skin on her face where adhesives were applied to hold her ng tube and nasal cannulas in place would break open and blister within a couple of hours. All of her wounds were a potential source of infection which was another concern to the transplant centers.
In order to help prevent the body from rejecting the transplanted organ, patients are given powerful immunosuppressant medications. This regimen substantially cripples the body’s ability to fight infection. While post transplant children are on these medications for life, the highest doses are given during the first few years post-transplant.
During the phone call, Dr. Carlson let us know that Rini’s prealbumin had reached 11.0, but with her better nutritional and weight status, her respiratory function had decreased, she was coughing, vomiting, and fluid balance was becoming increasingly problematic. They had introduced a third diuretic to combat the edema. Her ventricular function had shown no improvement with her nutritional gains and in fact had decreased. Her ejection fraction (amount of blood squeezed out of the ventricle with each heartbeat) was hovering around 10-12%. A normal EF is between 50-70%, with “severely depressed” beginning at less than 20%. The lower the EF, the higher the risk there is of life threatening arrhythmias and sudden cardiac death. And in Rini’s case, because her heart muscle was severely thickened and stiff, the actual amount of blood that entered her ventricle was less than normal to begin with.
The distant hope we had all held onto that metabolic stability might bring improved cardiac function, enabling the first of many surgeries she would need to take place, was firmly extinguished.
Dr. Carlson proposed Eric and I begin looking into the heart failure/transplant program at Seattle Children’s Hospital. She had been a Cardiac Fellow with their transplant team, and the cardiologist who was now in charge of the program had once worked at the very hospital where Rini was. Dr. Carlson said that she had already spoken to the Seattle team and they would be reviewing Rini’s records on the 11th. They gave her a tentative date of Monday, October 14th for their decision regarding her candidacy for transplant evaluation.
You might be wondering why a transplant center wouldn’t automatically give a child in need a chance. There’s nothing to lose, right? How could anyone turn away a dying child?
Over the next two weeks, we would get a crash course in the complex ethical conundrum that is transplant listing and organ allocation, and our perception of the term “supply and demand” would be forever altered.


























Leave a Reply