Read this blog about a family who has adopted a child with hemophilia:
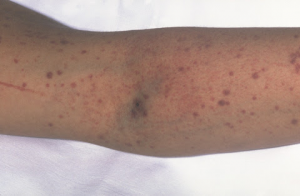
Hemophilia is a rare bleeding disorder in which a person’s body does not make enough of one of the proteins (clotting factors) necessary for blood to clot effectively. This means that individuals with hemophilia bleed longer than a typical person, but they do not bleed faster than others. Thus, children with hemophilia bruise more easily than other children, and may experience more mouth and nose bleeds than other children. Health concerns include joint bleeds and intramuscular bleeds that can cause joint and muscle damage. Internal bleeding and intracranial bleeds can be life threatening. These concerns can be managed with treatment.
Hemophilia is genetic and is most common in boys, though girls can carry the gene and can, on rare occasions, have hemophilia, too. Girls who carry hemophilia can also have symptoms.
The most common type is Hemophilia A (Factor VIII deficiency) with three levels of severity:
– Mild (5-50% of normal Factor VIII levels)
– Moderate (1-5% of normal factor VIII levels)
– Severe (less than 1% of normal Factor VIII levels)
A person’s level of clotting factor typically does not change throughout life, so a child’s severity level will likely remain constant through his or her lifespan. The most common treatment is factor replacement therapy, which is when concentrates of the missing clotting factor are infused into the bloodstream intravenously (either into a vein or through a port, depending on the treatment route a family chooses). Children who have mild and moderate hemophilia are typically treated “on demand” and clotting factor is infused when needed to treat a bleed or injury. The standard of care for children with severe hemophilia is prophylactic clotting factor replacement, and they receive infusions of their missing protein on a regular schedule of two, three, or more times per week.
Sometimes, a rare complication of hemophilia arises when a person’s body develops antibodies to the clotting factor infused in replacement therapy, rendering it ineffective in supporting clotting; this is called an inhibitor, which can be managed with treatment. Infusions take very little time, so life for a child with hemophilia looks much like that of any other child. They can go to school, participate in sports activities (contact sports are strongly discouraged), run, and play like other children. Without treatment, the life expectancy for a person with hemophilia is about 24 years. However, with proper treatment a person with hemophilia lives a typical, full lifespan.
Resources:
Kelley Communications
Hemophilia Mother Facebook Group
Adopting a Child with Hemophilia
Love Without Boundaries: Adopting a Child with Hemophilia
Adopted Into Hemophilia
Infusing Love
National Hemophilia Foundation’s Steps for Living
Hemophilia Adoption Facebook Group
Read blog posts about Hemophilia on No Hands But Ours.