Visit the following blogs to read about families who have adopted children with Congenital Nevus:
Growing Beards
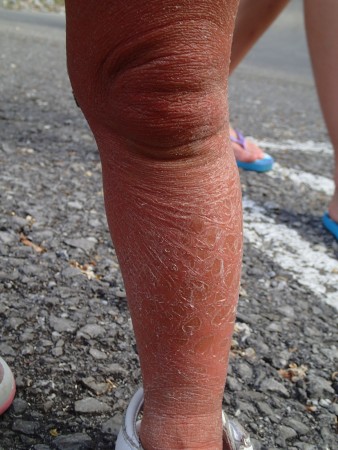
A Congenital Melanocytic Nevus can sound like an overwhelming special need. Simply, it is a birthmark (Nevus) present at birth (Congenital) that is made up of melanin or pigmented cells (Melancytic). Congenital Melanocytic Nevus (CMN) develops in the first trimester of fetal development and is NOT considered to be a hereditary or genetic condition. A nevus is often described based on the size of the birthmark: small, large, or giant. A large nevus covers more than 2% of the child’s skin, measures over 8”, would require more than one surgery to remove, or covers a large area of a body part such as an arm or leg. A large nevus is rare occurring in only 1 in 20,000 births. It is also very common to have “satellite” nevi, or smaller birthmarks, on other parts of the body in addition to the primary nevus.
There are some medical risks attached to this special need beyond the birthmark itself. An MRI is recommended to rule out a condition known as Neurocutaneous Melanocytosis (NCM). Individuals born with a large CMN have a 7% chance of having melanocytes (nevus cells) in their brain or spinal cord. More than 60% of those 7% of individuals with NCM, do not have any medical complications, even though an MRI conformed the presence of melanocytes in their nervous system. Complications from this condition may present as fainting, eyesight issues, hydrocephalus, or seizures.
Another risk is Melanoma, an aggressive form of skin cancer. Individuals born with a Congenital Melanocytic Nevus have a slightly elevated risk of Melanoma over the general population. It is estimated that a person born with a large nevus have a 2-5% chance developing Melanoma in their lifetime. An average person has a risk of Melanoma around 1% so current research estimates that an individual with a large, Congenital Melanocytic Nevus only has a slightly higher risk of developing this aggressive skin cancer. It is currently unknown if surgical removal of the nevus actually lowers the future risk of developing Melanoma.

With the unique needs and trauma involved in orphan care and adoption, it is important to evaluate the attachment and emotional needs of your child before committing to medical and surgical procedures that are non life-threatening. It is recommended to visit a pediatric dermatologist every 6 months for follow-up and evaluation.
A dermatologist can to determine if removal is necessary and other treatment options available. The decision to surgically remove a nevus is a highly debated, personal choice. If a family chooses to pursue removal, you would want to seek the opinion of a plastic surgeon in your area. Many Nevus families also chose to consult Dr. Bruce Bauer, Chicago, IL.
In recent years, the most common surgical removal option for a nevus is tissue expansion. Tissue expansion involves one surgery to place an expander (or multiple expanders) under the patient’s skin, expanding it over time with saline like a balloon, and stretching the skin to replace the nevus skin during a second removal surgery. It is fairly common for a patient to go through several rounds of expanders and removal surgeries to remove a large nevus.
Resources:
Nevus Outreach
Congenital Nevi
Giant Congenital Nevus
Giant Congenital Melanocytic Nevus
Nevus Love FB Support Group
Nevus Outreach FB Support Group
Read blog posts about Congential Nevus on No Hands But Ours.