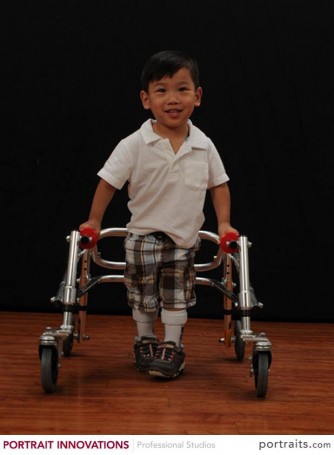
Visit these blogs to read about families who have adopted a child with Cerebral Palsy:
The Little Girl in Pink
Adoption Adventure with Two Little Princesses … AND Princes Two!
The Hameloth Family Journey
Orphaned No More
Cerebral palsy, also referred to as CP, is a term used to describe a group of chronic conditions affecting body movement and muscle coordination. It is caused by damage to one or more specific areas of the brain, usually occurring during fetal development; before, during, or shortly after birth; or during infancy. Thus, these disorders are not caused by problems in the muscles or nerves. Instead, faulty development or damage to motor areas in the brain disrupt the brain’s ability to adequately control movement and posture.
“Cerebral” refers to the brain and “palsy” to muscle weakness/poor control. Cerebral palsy itself is not progressive (i.e. brain damage does not get worse); however, secondary conditions, such as muscle spasticity, can develop which may get better over time, get worse, or remain the same. Cerebral palsy is not communicable. It is not a disease and should not be referred to as such. Although cerebral palsy is not “curable” in the accepted sense, training and therapy can help improve function.
Resources:
American Academy for Cerebral Palsy and Developmental Medicine: Although the primary purpose serves to educate the health care professionals and providers who treat and care for those with cerebral palsy and developmental challenges, it also gives the latest information and resources to families and parents.
United Cerebral Palsy: Connects families with information and resources both on the web and in their state.
CP Hope Through Research
CDC Cerebral Palsy
Adopting a Child with CP (video)
CP Daily Living: A website with a rich source of information about day to day care of a child with CP. It covers insurance information and resources, state by state resources, book reviews, therapy, assisted living equipment, general information, FAQ and more.
International Alliance for Pediatric Stroke
Canine Companions for Independence
Children’s Hospital of St. Louis
Cerebral Palsy Source
Cerebral Palsy International Research Foundation
My Child without Limits: A nonprofit organization that’s mission is to provide education and resources to families facing the day to day challenges. It includes a wealth of resources, glossary of terms often associated with specific health challenges, medications, procedures and more.
My Child at CerebralPalsy.org
Humanitarian Foundation (dental care for children w/CP and other neuromuscular disorders)
Friendship Circle
March of Dimes
Types of Cerebral Palsy
Reaching For The Stars
Books:
Cerebral Palsy: A Complete Guide for Caregiving, by Freeman Miller & Steven Bachrach
Teaching Motor Skills to Children With Cerebral Palsy And Similar Movement Disorders: A Guide for Parents And Professionals Paperback – July 19, 2006
Too Loud, Too Bright, Too Fast, Too Tight by Sharon Heller, Ph. D
Raising a Sensory Smart Child: The Definitive Handbook for Helping Your Child with SensoryProcessing Issues by Lindsey Biel and Nancy Peske (Aug 25, 2009)
The Out-of-Sync Child by Carol Kranowitz and Lucy Jane Miller Ph.D OTR (Apr 4, 2006)
Programs in the US available to Families with Special Needs:
Early Intervention: You will find a great description of Early Intervention, the government funded program that provides in home therapy services for children 0-3 with special needs. It will give you direction to your state’s specific program and how to get the services your child can benefit from.
Facebook Groups:
Cerebral Palsy Parents Information
Cerebral Palsy Adoption
Selective Dorsal Rhizotomy – St. Louis Children’s Hospital
PVL Periventricular Leukomalacia
Parenting our adopted children with CP
Cerebral Palsy Support Group
Yahoo Groups:
Cerebral Palsy Club
Adopting Children with Cerebral Palsy
Cerebral Palsy Moms
Read blog posts about Cerebral Palsy on No Hands But Ours.