In 2011, we received the file of a little girl, age 3. Her file read “delayed mental development” and it included a very low DQ score. We were able to ask questions and receive a video of her reading flashcards and reciting the names of the items on the flashcards.

“Okay,” we thought. “Yes, she’s probably delayed, being in an institution for 4 years by the time we meet her. But from this video, it looks like she’s doing moderately well.”
We decided to take the plunge into our second adoption.
Fast forward 6 months, and we were in China to meet her. She had a very traumatic gotcha day, poor thing. In fact, it was so traumatic for all of us, that we have no pictures or video footage of our first meeting as a family of 4. We took her back to our hotel, where she promptly went into what I called a “catatonic state”. She sat on the floor and stared for hours, all while little tears flowed down her cheeks. It was heartbreaking! Needless to say, she hadn’t said anything, or even made any sounds except grief-stricken ones, since we met her.
Rewind a little bit… the day before we traveled to China, we received an email from our agency that said our little one was in the hospital. Oh, no! What could be the matter?! Apparently, she broke out into some kind of rash or like skin condition, and the caregivers at her SWI had taken her to the local hospital for treatment. Okay. So, not as serious as it could be. We were thankful.
Back to gotcha day. We did indeed see the “spots” on her face that she had been hospitalized for. Did some research, tried to translate the hospital’s notes, and discovered it was mollescum. Not so unusual on kids in orphanages. Easy to deal with, especially once we got home. However, another skin condition became apparent later on gotcha day that we had no idea of.
At one point, after we had been back in our hotel for a while, she indicated that she had to go potty. I helped her to the toilet, and since I didn’t know if she was truly potty trained or not, I was ready to help her if need be. When I pulled up her pants, I noticed a dark mark on one of her buttocks. I panicked for a second and though it was a streak of #2 that I had missed. When I went to wipe it, it didn’t come off. Upon closer look, it was a section of raised skin, several shades darker than the rest of her skin, and very rough to the touch. It was about 3ish inches long. Hmmm… I had no idea what this was, nor had we received any indication of it in her file.
At bedtime, while I helped her change into pjs, I noticed more sections of the same raised, dark, rough patches of skin. On her neck, in her armpit, across her chest, behind her knee…all on the same side of her body as the one I first saw on her buttock. I did not do any more research while in China. We focused on bonding with her as much as possible, and acclimating to a family of 4.
Once home, we took her to our family doctor, as we had done with our first child upon arrival home from China. He, of course, noticed the patches and really took his time examining them. He determined that since they were all on the same side of her body, they were called “linear sebaceous nevus”. The technical definition of nevus is: a birthmark or a mole on the skin, especially a birthmark in the form of a raised red patch.
Our doctor then went on to tell us that linear sebaceous nevus usually presented as a syndrome. A general internet search provided the definition of LSN: syndrome (LNSS) is a condition characterized by the association of a large, linear sebaceous nevus (type of birthmark) with a broad range of abnormalities that may affect every organ system, including the central nervous system (CNS). The nevus usually is located on the face, scalp, or neck.
Okay. We were kind of freaked out by that.
Syndrome? Affecting every organ system? Abnormalities?
What in the world was going on?
She did have a small nevus on her neck, so that worried us even more. Our family doc sent us to a dermatologist for the mollescum, and it was a good opportunity to discuss the nevus with him as well. He told us that normally nevus have to be excised, as they tend to grow back. And that if they didn’t bother our daughter, maybe we should consider just leaving them alone and take on a “wait and see” attitude. So that’s what we did.
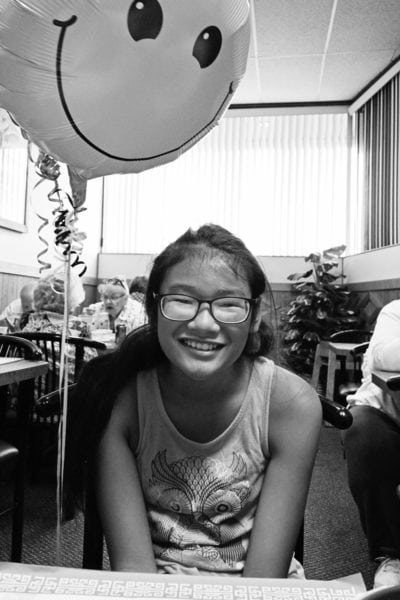
As we approach our 7th gotcha day anniversary, I have to be honest and tell you that these nevi have not affected our daughter negatively in any way whatsoever. I was worried especially about the nevus on her chest, as it could affect her decision to breastfeed one day, as well as affect her body image. But, as she’s developed, the nevus on her chest has “shifted” so that it’s not in the exact same spot as it was when she was little. Her other nevi have become less coarse over time, and have never bothered her – not even one day in her life.
As far as the syndrome goes… we still don’t know for sure. She definitely has speech/language delays. Is that related to the LSN? We don’t know.
Recently, she presented with a thyroglossal cyst. We are currently undergoing treatment for it. Is that related to LSN? We don’t know.

At this point, anything is possible. What we do know is that she is a creative, funny, athletic young lady of 11 years, who has a lot to offer this world. And we couldn’t love her more!
– guest post by Amy

























Leave a Reply