Rini, our youngest of six children, was adopted in August of 2013 at end stage heart failure stemming from complex, single ventricle congenital heart disease. She was admitted to the hospital immediately upon arrival home and within two weeks it was determined that she was inoperable, her only hope would come through cardiac transplant. She was initially found to be ineligible, but that would change thanks to a heart failure/transplant program that chose to take a chance on hope and optimism.
Much as we owe her life to the sacrifice made by her birth family in letting her go, we also owe it to the incredible, selfless act of organ donation made by a family in the midst of the incomprehensible loss of their child.
This series is a retrospective of the weeks leading up to Rini’s transplant which took place on November 13, 2013, and it is my hope that it will help to bring awareness to the importance of registering to be an organ and tissue donor.
We all have the power to be someone else’s miracle.
Donate Life!

From October 24th, 2016
On this day three years ago, Rini was officially listed for transplant. What an unbelievable moment that was for us! When Rini joined our family at end stage heart failure and was deemed inoperable, there was so little we could offer her. Hope was something we could offer, and that would come from transplant.
From my journal:
“Just about an hour ago at 3:00, the transplant coordinator arrived with the wonderful news that they are in possession of the official approval of transplant coverage from our insurance company, and she went over the forms for us to sign indicating our understanding of the transplant listing process. Eric said that he still can’t believe that we are here, in this space at this moment!

We talked and talked, and then we asked when Rini would be officially listed, and she said within half an hour of her leaving our room and going to her computer. We were like, “Well… GO!”
So as of this moment as I am typing, Rini is newly listed! She is listed 1A in Region 6. Because of her listing at the most critical status, her new heart will most likely come from this region since donor hearts are first offered to those at Status 1A within the region of the heart’s origin. However, a donor heart may come from outside of the region, from as far away as two thousand miles.
She told us all the details, and how they determine travel time by the winds aloft, how one of the transplant surgeons and nurses will travel by Leer jet to the hospital where the donor is, and will travel back with the heart. The elapsed time between clamping in the donor’s body to unclamping within the recipient’s can be no longer than 5-6 hours, no more than 3.5 hours of flight time, time for ground transport…. so much to think about, so many complex emotions.”

The intubation and the addition of more cardiac medications appeared to produce the desired effect. Rini was heavily sedated, and her heart was resting. For the first time ever, we saw her heart rate in the 120s. Her transplant cardiologists said that waiting a bit for a heart might be to her benefit, as they were very concerned about her weight and malnutrition. Her lowered heart rate, reduced work of breathing, and sedation would most likely assist her in gaining over the next weeks and months, which would give her reserves for the work of healing if she was a heart recipient.
Rini fooled us all. We thought she the luxury of time. How wrong we were.
From October 25th, 2016
On this day three years ago, I headed home to Oregon while Eric began his first two-week stretch at the hospital with Rini. Her sedation was lifted to check her responses to stimuli, and Eric sent me a photo so that I could see my baby’s eyes. Soon she began thrashing, so she was once again more heavily sedated.
Before I left, we went to a local store and picked out birthday decorations so that he could dress up Rini’s room for her special day two days later. It was important to me that her birthday be celebrated, even though she would not be conscious of it, and I felt desperately sad that I would not be there. When your child is so sick and survival is very uncertain, acknowledging each milestone takes on a particular importance.
I was also fueled by a determination to memorialize each step in her life so that I could share it with her when she grew up. And right there was that push-pull, that agonizing dance of alternately preparing for her death while planning for her future.
From my journal:
“It feels like it is either twilight or early dawn, and I don’t know which yet. The fall leaves are at their glory right now and as I admired our maples, I was hit yet again with that piercing realization that she isn’t here to enjoy this beautiful time of year, and how desperately I want her to make it through this and be home with us for next year’s autumn.”

From October 26th, 2016
On this day three years ago, Eric called me to tell me that the nursing team was preparing to move Rini to a different room. When Eric asked the reason, he was told, “We move beds here, we move beds there. We do this all the time.” Well, I wasn’t buying it. I kept picking on this topic throughout the day when Eric and I would talk, and then finally that evening, after Rini was settled into room 218, her nurse told him, “It’s because we want her as close as possible to the nursing station.” They also positioned her bed so that her head was closest to the room’s entrance.
At first I was perplexed as to why her caretakers did not simply say what was on their minds, which in this case would have been, “We are concerned that your daughter is going to go into cardiac arrest, and we want her in close proximity to us and positioned in such a way as to better facilitate life saving measures.” But as our time in the hospital stretched from days to weeks to months, I learned to read between the lines and came to understand that much is communicated in what is not said. I also came to appreciate why they often hold back from sharing certain information until their hands are forced.
Caretakers in an Intensive Care Unit have a tough job, and I don’t just mean caring for some of the most fragile children. I mean dealing with some of the most difficult parents. After witnessing firsthand how challenging and sometimes outright abusive families can be towards their child’s doctors and nurses, I have even more respect for the medical profession. After observing parents falling apart and teetering on the edge of hysteria (and sometimes going over the cliff) over relatively minor issues and becoming confrontational towards the very people attempting to save their children’s lives, I completely get why the doctors and nurses do not inform parents each and every time they are going to make an adjustment here and an adjustment there, or even when they have larger concerns but do not have empirical evidence of where the child may land. I had the experience of getting to know a mother whose daughter was admitted with heart failure, and whose take on the situation was that “…. my daughter is perfectly fine. They just want to cut on her.” Can you imagine trying to perform your job as a cardiac critical care nurse or cardiologist when confronted with that?
Eric and I learned a long time ago that medicine is as much art as it is science, and that when treating children with complex conditions, very rarely is there a roadmap. That was a jarring lesson to learn, and looking back I see that at one time I did believe that excellent doctors always knew the answer. It’s easy to default to the “they-must-be-incompetent” frame of mind when they don’t. Sometimes, there just isn’t an answer.
We did our best to remain levelheaded, and in my opinion there is no excuse for treating another human being with disrespect, no matter how stressed a person is. We wanted to be partners with Rini’s caretakers, to cooperate with and be welcomed as a vital part of her team. After we approached them and explained that we understood that sharing their thoughts with us did not equate to a commitment or a promise that the plan would yield the results we hoped for, more was shared. We came to enjoy an open dialogue and loved how we were embraced as collaborators in Rini’s care, listened to and respected during rounds, and consulted with. We developed a genuine affection for those who continue to care for her to this day.
October 26th, 2013 was also the day on which I began to obsess over all things related to Rini being listed for transplant. It became unhealthy, as it was symptomatic of my wanting to find some way to control the outcome. That was not sustainable and I would be forced to learn to let go.
Walking with Rini during that time was when I learned what faith is.
From October 27th, 2016
On this day three years ago, a very brave little girl turned 2 years old. The night before, Eric had texted me photos of the decorations he had placed on the outside of Rini’s room so that all who passed by could share in the celebration. When I picture my husband lovingly taping up her banner and other celebratory trappings, my eyes fill with tears thinking of him giving what he could to his daughter.
He had also gone to a local bakery and ordered her cake, which he placed in the ICU family lounge with a note asking the other parents to help us celebrate by enjoying a piece. And because he knew that I’d want an Asian princess on her cake, he had taken a black Sharpie to the blond figurine’s hair.

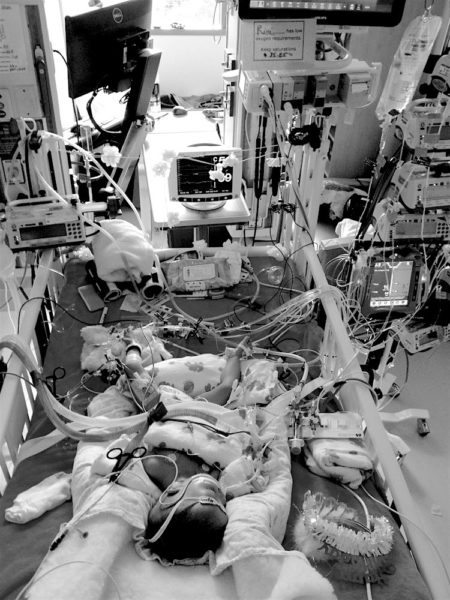
Rini’s scheduled medications were up to 14, and her p.r.n. meds were up to five. She tested positive for Haemophilus Influenzae which she was being treated for, and was receiving blood transfusions in order to maintain her hematocrit to improve her renal NIRS and tissue oxygen delivery. Rini’s feeding tolerance continued to worsen, she was switched to full TPN and intralipids nutrition, and she was characterized as “challenging to manage” in regards to fluids. I was used to seeing my children post cardiac surgery with many lines and illuminated medication towers, but as time went on, the entanglement grew less. With Rini, her decline was illustrated by its increase.
From my journal:
“Yesterday, they moved Rini from room 203 to 218, and every shift she will have a nurse that is unpaired (in other words, the nurse will only have Rini as her patient for the entire shift). The team is still working on stabilizing her for the wait. Finding the right balance of feeds, fluids, diuretics, and the cocktail of medications she is on remains challenging, and today they defined her status as “still fragile”. The hope is that they will be able to find that balance where she can remain and gain weight.
Although I have fought it since Wednesday, I have caved into the temptation to obsess over her transplant listing. There is a database patients and families can go to where you can see how many other children are listed in the UNOS regions and set up search parameters to include age, listing status, accrued wait times, blood type, etc. As I felt solace to see for myself what her team had commented on regarding her being the only child listed in her weight class and with her blood type, I concurrently felt morbid in my relief given the hard truth of where a healthy heart will come from. Eric and I are both struggling with being in this space.
And as our third official day of waiting comes to a close, I was struck by how in many respects it feels like when we were waiting for our first child referral from China back in 2006, with obvious differences of course. But the reality that we have gained five of our children only through other families’ losses resonates.
On the home front, I can feel that my relationship with our other children has changed. I am now feeling that I am becoming the mother I have wanted to be. Bluntly, I am far more patient. I am relishing every hug and smile, and tonight after bath time I found myself smiling and enjoying the process of rubbing lotion onto their little feet and faces, clipping their nails, and brushing their hair. What I wouldn’t give to be able to do those things for Rini right now, and to be able to hold her close and hear her voice. Eric said to me that he is determined to “make this time count”, and I couldn’t agree more. Although it sounds counterintuitive, the stress has, I believe, brought about a new clarity.
I am grateful to have the most steadfast and true friends that I am able to turn to with my most painful feelings, my guilt, regrets, and my desperation. And how fortunate I am to be surrounded by wise women who share their experiences and perspectives. A few days ago, a friend who is in a similar situation counseled me to find my peace with letting Rini go. It reminded me of when I posted my disagreement with the idea that “life equals winning and death equals losing”. Her words were of such comfort because on that very day, I had come to a place where I realized that I have to let go and find a place of acceptance with whatever is to come. With that came some guilt, as though by embracing the idea that Rini still wins in death (after all, she will be in Heaven if that occurs), I was giving up the fight.
I am not giving up the fight, but rather understanding that I am not in control.
I can advocate for her the best I can, and those caring for her can do their utmost, but in the end, it will be what it will be. And I firmly believe that my role will be to find some type of meaning and even if I am not able to find it, to have the faith that meaning exists.”
I prayed that Rini could feel our love for her on her special day. Happy Birthday, my sweet baby.


























Thank you so very much for sharing this heartbreaking, beautiful story. I haven’t commented before, but have really been moved by Rini’s story and look forward to each installment. Thank you again for sharing how you felt during this season of your life.
Thank you so much for reading, Danaile!