When my husband and I first were matched with our son, Jet, we didn’t know a whole lot about the world of pediatric cardiology and congenital heart defects.
Our son was born with heterotaxy (complete abdominal situs inversus) with left atrial isomerism, functional polysplenia, interrupted inferior vena cava, partial endocardial cushion defect, tricuspid and mitral valve defects, pulmonary hypertension, and a single/common atrium — of which the majority were repaired or improved with surgery in China thanks to the gift of hope from Morning Star.
But CHD is rarely a one and done surgery; it’s a lifelong battle of bravery and strength for the individual, their families, and their medical team.

So once we had his file we did our due diligence and consulted with our local children’s hospital, the Children’s Hospital of Illinois (CHOI), which happens to have an actual CHD clinic. We called on a Friday in March 2016 just before closing, and one of the doctors agreed to meet with us the following Monday after hours to interpret the file so that we would know what sort of treatment plan, if any, would be needed to submit our Letter of Intent.
We took the information we learned, wrote our LOI, and did what many adoptive parents recommend at that point: hoped for the best. The fact that we had a complete care CHD clinic not even fifteen minutes away from our home was entirely lost on us. At that point, we were just happy to have actual facts and data (my husband is an engineer) explained to us. We were entering into this whole new world, and didn’t realize how consuming it could be.
My goal is not to make this post about Jet (although indirectly it is because without Jet we wouldn’t know them) but instead about these very special people in our lives.
We came home in June 2016, and since we’ve been home, we’ve seen the cardiologists more than we’ve seen our own families, and that’s no exaggeration. (To be fair, our family is not local. My mother and mother-in-law I’m sure would want you to know that.)
For a while, his primary cardiologist was calling almost on a weekly basis with whatever new test results or updates he had on Jet when we first came home. Since then, we’ve had numerous tests and procedures, like a liver/spleen function test and abdominal ultrasound, Holter monitors, EKGs, echos, office visits, an MRI, multiple hospitalizations, one heart catheterization with stent placement, one open heart surgery with a bonus surgery a few days later, a pacemaker, and medications changed, added, subtracted, and then added again. We know our every six month visits that we recently graduated to will someday go back to every three, and then possibly every one month. We know Jet will need surgery again.
There is no “maybe”. It’s a fact.
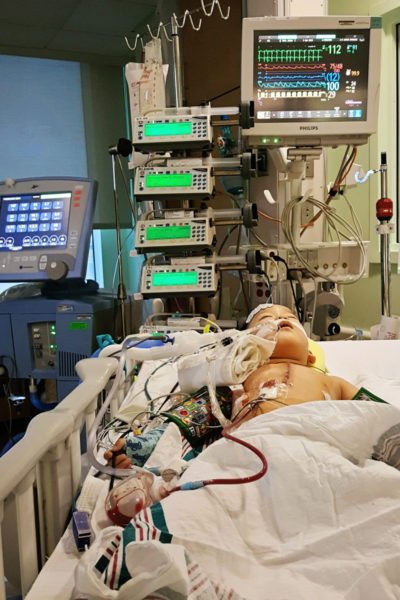
We’re still by no means experts, but what’s important is that we trust our experts, with our son’s actual life. And that’s no small feat.
When you bring home your child with CHD, you may already have a plan in place with a cardiologist that has reviewed the file, especially if your child is unrepaired or in need of immediate intervention. Jet was medically stable because again, most of his repairs were already done, so we had time. Of course, we started with the CHD clinic at CHOI where we had his file originally reviewed, but after we were home we still did our research.
We asked questions on social media, and made friends with other heart families. We looked at the US News Report for best hospitals with pediatric cardiology programs. We looked at our hospital and other hospitals’ STS (Society of Thoracic Surgeons) scores. We read up on Jet’s cardiologists: where they went to school, where they did their fellowships, what their specialties are, where their interests lie, etc. We looked at other cardiologists and at their credentials, and compared. And finally, last but not least, we looked at Jet’s needs, both in the short and long term.
Everyone has their own ways of finding care, and I know we could have found another hospital that would meet Jet’s needs, but we knew that the team of doctors here on Jet’s case were more than capable.
Yet, there were other factors that made us stay with our cardiologists. Like the time we weren’t even home a month, when his primary cardiologist called to update/confirm some test results. After he finished, he asked me how Jet was settling in, and really wanted to know the answer.
Or when, a few months later, Jet had his heart cath, the doctor who performed the cath gave him a piece of chocolate and two bowls of ice cream, because that’s what every kid needs when they just wake up from anesthesia.
Or when, waiting for our discharge papers the next day, this same doctor took him around and helped him decorate a Christmas tree.

Or knowing all that when the cardiologists were conferring about surgery for Jet, and ultimately deciding the benefits did not yet outweigh the risks and did not want to operate on a child if it wasn’t absolutely necessary.
Or that our cardiologist sent off Jet’s information to another hospital for consultation, just to make sure all i’s were dotted and t’s crossed.
Or when the same cardiologist stopped in to say hi and chat after clinic hours were done for the day during one of Jet’s hospitalizations because of trouble breathing, even though he needed to get home because he promised he’d take his kids to see the new Star Wars.
And we can’t forget the nurse who held Jet’s hand all the way from the clinic to the lab for blood draws.
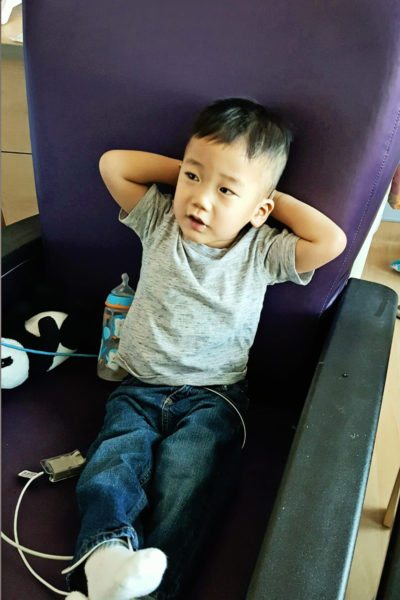
And then, when Jet finally did need surgery, it was delayed for a week because his pre-op testing came back with not optimal results, and our cardiologist called, from vacation, to say he was so sorry the surgery was delayed, but he was selfishly glad that he would be there, because Jet was one of his kids.
It was when the surgeon, five days after doing Jet’s open heart surgery, was at the hospital within a half hour of test results showing a complication, who reassured us he would find the issue (and he did).
It was the surgeon’s APN, who at Jet’s one week post-op appointment, looked at me with tears in her eyes, telling me how hard it was to see him just wanting to be held but because of all of the tubes and wires and IVs and drains there was no way.
It was the nurse, who gifted Jet with a PomPom (panda), his favorite animal that now proudly sits in his collection of pandas known as “Nurse PomPom.”
It was six weeks post op, when we were taking our required photos for our one year post adoption report, and I snapped a picture of Jet with his #squadgoals medical team, all of the people who work together to give our son the best care possible.

There’s no way they could know what these small, trivial snapshots in our memories mean to us; these instances that proved not only do they love what they do and that they are good at it, but that they genuinely care for Jet.
About six months after we were home, we were driving to the hospital and when we came down the hill toward the parking garage, Jet started shouting “Doctor friends! See doctor friends!” We never told him to call them our friends. Of course we affirmed and encouraged the knowledge that doctors are here to help us feel better, but Jet came up with them being his friends all on his own.
To us, as his parents, knowing that he loves and feels comfortable with his doctor friends is a testament to them, that even at only two years old he knew they’d take care of him. In fact, it’s been almost a year since Jet’s surgery and every time we go past the hospital (because it’s on the way to the coffee shop #priorities), we still have to wave and say hi to our doctor friends. The knowledge now that we live so close to a comprehensive congenital heart care center does not escape us; only God could have orchestrated that. Every family needs to choose and do what is best for their child, and we’re so thankful for all these instances, along with the quality of care, made it clear that we’re where we need to be.
I hope you also find your own doctor friends, whether you have a home team, an away team, or both.
– guest post by Mary: email || blog || instagram

























Leave a Reply